 Communication Everywhere All at Once–the Art of Leveraging TechIn medical school and residency, the emphasis on medical knowledge often overshadows other equally important aspects of effective patient care. At some point, the hard realization hits that just knowing and understanding the literature is not enough. Without medical knowledge matched to excellent communication skills, our knowledge is unavailing. Strong communication skills are foundational to ensure a multidisciplinary care plan is carried out by consultants, nurses, social workers, and physical therapists. High-quality communication between the care team, patients, and their caregivers can prevent medical errors and decrease readmissions. Unfortunately, in the busy, stressful life of a hospitalist, our day-to-day tasks can take precedence over the basic and powerful notion of being a good listener.
Communication Everywhere All at Once–the Art of Leveraging TechIn medical school and residency, the emphasis on medical knowledge often overshadows other equally important aspects of effective patient care. At some point, the hard realization hits that just knowing and understanding the literature is not enough. Without medical knowledge matched to excellent communication skills, our knowledge is unavailing. Strong communication skills are foundational to ensure a multidisciplinary care plan is carried out by consultants, nurses, social workers, and physical therapists. High-quality communication between the care team, patients, and their caregivers can prevent medical errors and decrease readmissions. Unfortunately, in the busy, stressful life of a hospitalist, our day-to-day tasks can take precedence over the basic and powerful notion of being a good listener.
With technological advances, modern communication practices have added more opportunities and associated challenges. Video calls are now routinely used to communicate with patient’s families, and patients have direct access to their medical records in real-time. Electronic health records (EHRs) have integrated chat features with resultant workplace communication now at risk of mimicking casual texting patterns. As technology changes, the practice for inpatient providers must adapt, and the fundamentals of communication and careful listening must remain.
Video calls at the bedside
It’s estimated that 90% of communication lies in the nonverbal and paraverbal components—how we use body language, gestures, facial expressions, and the tone and volume of our voices.1 Nonverbal communication can significantly impact patient satisfaction, outcomes, and the likelihood of adherence to the recommended care plan.2 Communicating information to patients should resemble a conversation we have with loved ones. We must confer empathy, show interest in a patient’s story or questions, and ensure we are patient and avoid interrupting.1
Technology has both helped and hampered this ability as we have been pushed to spend more time with the EHR and less with the patient.3 As hospitalists, we often try to multitask, calling our patients and caregivers on the phone and updating our patient’s families while writing notes.4 This can lead to distracted conversations and less engagement and active listening. The use of video calls has grown exponentially with the COVID-19 pandemic. Video calls have been shown to reduce loneliness and isolation for the geriatric population and improve connections between patients and mental-health providers.5,6
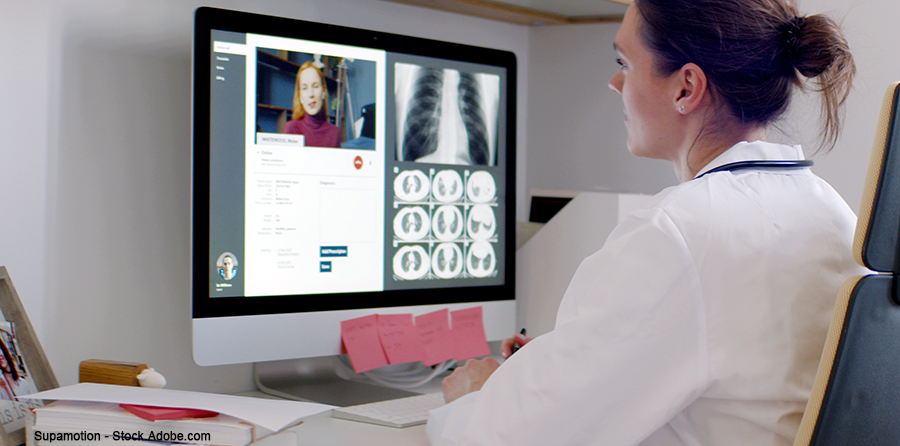
During the pandemic, many hospitals expanded the use of tablets on the wards to allow for video calls for consultants and family members. Some EHRs have integrated the feature, as have smartphone apps for physicians, like Doximity. Helping a patient set up a video call to connect to their family can be invaluable, providing the connection needed to allow for the nonverbal and paraverbal elements of communication. When it comes to breaking bad news, it can allow for the needed silence to let families process and permit physicians to watch for nonverbal cues to ensure understanding. Video calls can be made in a patient room to allow for a hold or pat on the shoulder that a distant family member cannot provide.
Open access to health information
Though this existed well before COVID-19, the pandemic embroiled us in a world where disinformation became as prevalent as good information and people became self-proclaimed experts by doing their own, sometimes limited, research.7 The medical community responded with sarcastic memes about confusing a Google search with a medical degree. As access to information has expanded over the last two decades, the amount of information patients bring to encounters has increased and is likely to grow more as artificial intelligence enhances patient research.
Good communication with patients and families involves integrating their input and ideas. Taking time to listen, even when the information challenges your care plan, is key to building a trusting relationship. We must avoid being adversarial and instead focus on slowing down, showing genuine empathy, and sharing our expectations for patient care with patients and family members.
Previously, patients did not have easy access to their medical records. With advancing technology and federal legislation, patients now can quickly view their lab results (sometimes before the clinician), including those flagged as abnormal.8 Health systems must partner with patients to find ways to ensure certain diagnoses (i.e., cancer) are not discovered by a patient alone when viewing results with limited context. We must advocate for continued direct communication in the timely delivery of bad news. Harm can also come when patients read notes that have stigmatizing language such as “difficult” or “non-compliant.”9 Clinicians must refine the language used in notes to eliminate stigma and understand more about why certain labels are short-sighted. We must presume that all of our notes are being read by our patients and their family members.
Secure messaging
Though it’s easy to forget in the era of constant notifications, secure messaging has been viewed favorably by hospitalists as an improvement in clarity and efficiency.10 Secure messaging on a pediatric hospitalist service resulted in a 59% decrease in communication failure between nurses and residents but was accompanied by increased messaging rates.11 Secure messaging provides many benefits but has drawbacks including lack of standardization, confusion on whom to contact, and risk of alert fatigue.
Successful communication in the era of secure messaging relies on clear rules of engagement about whom to get in contact with and when and how to do so. Health care systems must establish conventions, with all stakeholders involved in patient care providing input. Specifying approaches for urgent- or emergent-care needs is imperative. Alternative communication options must remain, including pagers, phones, and/or overhead paging to provide a backup and an emergent response system. Clear pathways and expectations on communication type can promote efficiency while ensuring closed-loop communication. When clinicians go off service, there should be standard practice to change the contact person and make the outgoing clinician unavailable to avoid communication delays.
It is too easy to be informal in secure messaging which can lead to miscommunication and multiple unneeded messages back and forth. Messaging must follow existing standards, such as Situation, Background, Assessment, and Recommendation (SBAR) or other validated communication tools. Clinicians should set an example by using one message in an SBAR format rather than multiple fragments that increase alert fatigue. High-quality direct communication on multidisciplinary rounds, recognizing quickly when a return to the bedside is needed, and clarifying complex issues verbally (by phone or in person) can decrease the messaging burden.
For now, we encourage hospitalists to understand the importance of communication, with a distinct focus on how to leverage technology to help us, including how to videoconference to update families, how to ensure the medical record is patient-focused and patient-friendly, and how to secure-chat professionally. Technology will continue to change rapidly, and hospitalists will often be at the forefront to see its potential to improve care while also appreciating its flaws and shortcomings. As technologies advance, we must stay up-to-date to ensure that the changes of the future positively impact outcomes for our patients and assure a heightened sense of pride in our day-to-day careers extending far beyond checking the boxes of our future HospitalistGPT-created to-do lists.
SHM’s Physicians in Training committee shares articles on topics relevant to trainees and early-career hospitalists.

Dr. Perry

Dr. Sansbury

Dr. Hall

Dr. Molitch-Hou
Dr. Perry is an internal medicine-pediatrics resident at Indiana University in Bloomington, Ind. Dr. Sansbury is the transitional-year program director, internal-medicine associate program director, chair of the department of medicine, and medical director of the Grand Strand Health Education and Simulation Center at Grand Strand Health in Myrtle Beach, S.C. Dr. Hall (@AlanHall_UKHM), is an associate professor and hospitalist in internal medicine and pediatrics at the University of Kentucky College of Medicine in Lexington, Ky., where he also serves as the assistant dean for curriculum integration. Dr. Molitch-Hou (@EthanMH3), is an assistant professor, director of hospital medicine sub-intern rotation, and co-director of the Care Transition Clinic at the University of Chicago Medical Center in Chicago.
References
- Ranjan P, et al. How can doctors improve their communication skills? J Clin Diagn Res. 2015;9(3):JE01-04.
- Choudhary A, Gupta V. Teaching communications skills to medical students: Introducing the fine art of medical practice. Int J Appl Basic Med Res. 2015;5(Suppl 1):S41-44.
- Asan O, et al. More screen time, less face time – implications for EHR design. J Eval Clin Pract. 2014;20(6):896-901.
- O’Leary KJ, et al. How hospitalists spend their time: Insights on efficiency and safety. J Hosp Med. 2006;1(2):88-93.
- Noone C, et al. Video calls for reducing social isolation and loneliness in older people: a rapid review. Cochrane Database Syst Rev. 2020;5(5):CD013632. doi: 10.1002/14651858.CD013632.
- Molfenter T, et al. Use of telehealth in mental health (MH) services during and after COVID-19. Community Ment Health J. 2021;57(7):1244-51.
- Levy N. Bad beliefs: Why they happen to good people. Oxford (UK):Oxford University Press;2022. https://www.ncbi.nlm.nih.gov/books/NBK577958/. doi:10.1093/oso/9780192895325.001.0001. Accessed December 31, 2023.
- Krasowski MD, et al. Variation in results release and patient portal access to diagnostic test results at an academic medical center. J Pathol Inform. 2017;8:45. doi: 10.4103/jpi.jpi_53_17.
- Sun M, et al. Negative patient descriptors: Documenting racial bias in the electronic health record. Health Aff (Millwood). 2022;41(2):203-11.
- Przybylo JA, et al. Smarter hospital communication: Secure smartphone text messaging improves provider satisfaction and perception of efficacy, workflow. J Hosp Med. 2014;9(9):573-8.
- Hansen JE, et al. Reducing interdisciplinary communication failures through secure text messaging: A quality improvement project. Pediatr Qual Saf. 2018;3(1):e053. doi: 10.1097/pq9.0000000000000053.