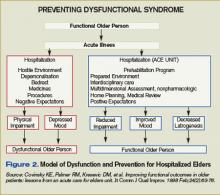
Each patient’s assessment is multidimensional, with an emphasis on nonpharmacologic interventions where practical. For example, an emphasis is placed on after-dinner exercise such as walking and socializing to promote sleep and reduce medication use. Nursing-care plans were revised to promote mobility, discourage inappropriate Foley use, and encourage adequate hydration and nutrition.
Recommendations are communicated to the primary team via a recommendation form placed in the physician-order section and text pages. The unit’s medical director and pharmacist review medications. Recommendations that involve medication changes are discussed with the primary team, which write all medication orders. Home planning begins on the day of admission.
Prior to opening the unit, the ACE unit social worker met with key city and county agencies including Aging and Adult Services, the Public Guardian, In-Home Supportive Services, and community nursing homes to introduce the unit and plan for an effective and safe transition.
All staff expect patients to maintain prehospital physical functioning. When possible, patients are expected to wear their own clothes, eat all their meals in a common dining room, and ambulate or exercise daily.
We considered establishing criteria for admission.13 We have not adopted formal criteria for patients 65 or older, presence of medical non-surgical condition(s) that require(s) acute hospitalization, and no need for telemetry or chemotherapy. As we learn how best to serve our hospitalized older adult population with the resources of the unit, we will re-evaluate targeting criteria. Most of our admissions are from the emergency department (ED), and the remainder are from other units in the hospital.
Challenges
Key challenges in opening the new service include securing commitment and resources from organizational leaders and key stakeholders; incorporation of the ACE unit concept in an academic training center; hiring key staff, especially the geriatric clinical nurse specialist and pharmacist positions; and completing the environmental rehabilitation on a limited budget.
While gaps in the care of the geriatric patient population were well identified at SFGHMC as far back as 1996 by a multidisciplinary task force, no actions on recommendations were taken, for several key reasons.
First, an executive level administrator or physician champion was not a member of the task force. Second, the organization did not have a department or regulatory mandate to address the gaps in the care of the elderly patients. Third, there was no link between the hospital strategic plan and the recommendations.
By 2004, these issues were largely addressed. A new chief nursing officer with a background in quality improvement understood the demographic and quality imperatives to improve care for hospitalized older adults.
That same year, the Hospital Executive Committee incorporated patient safety into the hospital strategic plan. This resulted in a successful business plan for an ACE Unit and geriatric consultation service linked to organizational strategy.
Funding was allocated for a medical director and a clinical nurse specialist in fiscal year 2005-2006. In addition, a grant was obtained from the SFGH Foundation to fund equipment, renovations, and staff education/training.
The original ACE unit concept involved expert, interdisciplinary geriatric assessment and communication of suggestions via a paper-based chart.
Initially, we felt the primary medical team should round with the ACE team, preferably at the bedside. However, informal focus groups held with the residents suggested this would happen infrequently.
The demands on the medical teams of completing patient rounds before morning attending rounds were cited as the main reason that model wouldn’t work.
We have implemented the following methods to promote communication between the ACE unit team and the primary medical team: