Families often note that after older relatives return home from the hospital, something is wrong with them.
While the acute condition that brought a relative into the hospital has been remedied, major functional and cognitive deficits such as confusion, falls, and difficulty with basic activities of daily living remain.
This post-hospital decline may not be appreciated by hospital clinicians, perhaps because the problems do not become visible until the patient is home. However, these problems place significant burdens on patients and families.
Following discharge for an acute hospitalization, about a third of older patients will have a major new disability that threatens their ability to live independently.1 Among community-dwelling elders, half of all new disability occurs within a month of hospitalization.2 It isn’t surprising that nursing home placement has grown more common for medical hospitalizations, even for seemingly reversible medical problems.
Older adults will make up an increasing number of the patients cared for by hospitalists. The Acute Care for Elders (ACE) unit model of care focuses on preventing functional decline and increasing discharges to home.
In 2005, leadership of the San Francisco General Hospital Medical Center (SFGHMC) committed to improving care for hospitalized elders by adopting the ACE model.3
The ACE model combats hospital-acquired disability by improving care processes for older patients.
Major motivating factors for the change included demographic and quality-of-care imperatives. After a nine-month planning process, the SFGHMC ACE unit opened in February.
Rationale
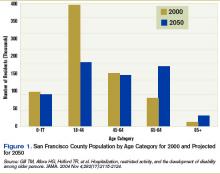
Largely driven by the baby boom, the number of California seniors older than 65 will double from 3.5 million to 7 million over the next 40 years, and those older than 85 will triple from about 500,000 to 1.5 million. In San Francisco, changes will be even more dramatic as the number of residents over 65 increases from 14% of the population to 32%.4 (See Figure 1, right).
In California, people 65 to 84 are almost three times as likely to be hospitalized as those between 45 and 64. If rates of hospitalization do not change, an increase in hospitalized older adults will occur as the baby boom generation ages.
In addition, hospitalization can be hazardous for older adults, with increased risk for functional and cognitive disability and adverse events.5-7 As a result, hospitalization-associated disability represents a growing threat to the independence of the older population. A variety of changes to usual care have been adopted in an effort to reduce the hazards of hospitalization in the elderly.8-11
ACE Model
The ACE unit model, proven to reduce the risk of hospital-acquired disability in the elderly, is based on the Model of Dysfunction for Hospitalized Elders.12 (See Figure 2, p. 23)
This model outlines how processes of hospital care for the elderly promote physical impairment and depressed mood, leading to dysfunction. Counterproduc-tive factors in older adults include a hostile environment (lack of natural sunlight, high-glare floors, poor way-finding cues, high noise levels), depersonalization (lack of personal effects, clothing, and usual daily routines), bed rest through multiple tethers or inattention, medicines inappropriate in the elderly or given at inappropriate doses, procedures, and negative expectations (usually that the patient will require nursing home placement after admission).
These processes are the targets of the ACE intervention. The idea is to improve quality of care for the elderly by promoting rehabilitation and preventing disability.
The ACE unit addresses these issues through a “prehabilitation program.” The ACE unit is a physical location in the hospital with 10 beds. Care is redesigned by placing the patient at the center of restorative efforts of an interdisciplinary team consisting of an advanced practice nurse, a social worker, an occupational and a physical therapist, a nutritionist, a pharmacist, and a medical director. This ACE Unit team meets daily to review and plan care for all patients. Recommendations for nursing care and rehabilitation evaluation are implemented by the ACE team directly. Other recommendations, such as changing medications or considering alternative approaches to common geriatric syndromes are communicated to the primary team, which maintains overall responsibility for the care of the patient.