We thought they were gone, but they’ve returned: diseases once considered “vintage bugs” that were common in as late as the mid-20th century. In the past these diseases killed one in three people younger than 20 who had survived an infancy during which many of their contemporaries died.1
“When you think about disease states, you think about some that are gone from the world,” says Erin Stucky, MD, a pediatric hospitalist at the University of California, San Diego, “but there are very few truly gone from the world.”
Some of the major infectious diseases that hospitalists may [still] see are pertussis (whooping cough), measles, and mumps, but scarlet fever and varicella (chicken pox) also endure—not to mention those occurrences of polio around the country that epidemiologists and infectious diseases specialists are monitoring closely. Rickets, a vitamin-D-deficiency-related disease also thought to be a relic of the 18th century, is showing up in certain patient populations—and not exclusively in infants and children.
This is a crossover clinical issue, our pediatric hospitalists say, and thus one to which their hospitalist partners who treat adult patients must also remain alert.
Adapted from Hopkins RS, Jajosky RA, Hall PA, et al. Centers for Disease Control and Prevention. Summary of notifiable diseases—United States, 2003. MMWR. 2005;52:55. Source: Gregory DS. Pertussis: a disease affecting all ages. Am Fam Physician. 2006 Aug 1;74(3):420-426.
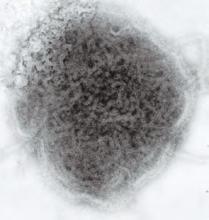
This negative stained transmission electron micrograph (TEM) depicts the ultrastructural features displayed by the mumps virus.
Adapted from Hopkins RS, Jajosky RA, Hall PA, et al. Centers for Disease Control and Prevention. Summary of notifiable diseases—United States, 2003. MMWR. 2005;52:55. Source: Gregory DS. Pertussis: a disease affecting all ages. Am Fam Physician. 2006 Aug 1;74(3):420-426.
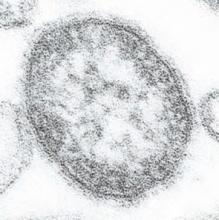
This thin-section transmission electron micrograph (TEM) reveals the ultrastructural appearance of a single virus particle, or “virion,” of measles virus.

Adapted from Hopkins RS, Jajosky RA, Hall PA, et al. Centers for Disease Control and Prevention. Summary of notifiable diseases—United States, 2003. MMWR. 2005;52:55. Source: Gregory DS. Pertussis: a disease affecting all ages. Am Fam Physician. 2006 Aug 1;74(3):420-426.
A photomicrograph of Bordetella (Haemophilus) pertussis bacteria using the Gram stain technique. Bordetella is a highly communicable, vaccine-preventable disease that lasts for many weeks and is typically manifested in children with paroxysmal spasms of severe coughing, whooping, and post-tussive vomiting (also known as Bordet-Gengou bacillus).
Adapted from Hopkins RS, Jajosky RA, Hall PA, et al. Centers for Disease Control and Prevention. Summary of notifiable diseases—United States, 2003. MMWR. 2005;52:55. Source: Gregory DS. Pertussis: a disease affecting all ages. Am Fam Physician. 2006 Aug 1;74(3):420-426.
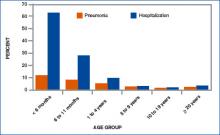
Figure 1. Number of reported pertussis cases by age group in the United States in 2003.
Source: Broder KR, Cortese MM, Iskander JK, et al. Preventing tetanus, diphtheria, and pertussis among adolescents: use of tetanus toxoid, reduced diphtheria toxoid and acellular pertussis vaccines recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2006;55:1-34.
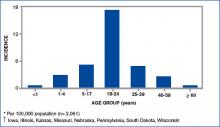
Figure 2. Incidence* of mumps reported in eight outbreak states, by age group — U.S., Jan. 1-May, 2 2006.
Source: Davenport ML, Uckun A, Calikoglu AS. Pediatrician patterns of prescribing vitamin supplementation for infants: do they contribute to rickets? Pediatrics. 2004 Jan;113(1):179-180.
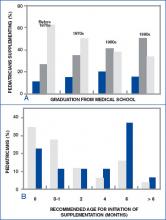
Figures 4A and 4B. Percentage of pediatrician practices for breast-fed infants, grouped by decade(s) of graduation from medical school.A: Recommending vitamins for none (black bar), some (gray bar), or all (white bar) infants. Note the high percentage of pediatricians who graduated before 1970 and who recommend vitamins for all breast-fed infants in comparison to those who graduated more recently.B: Recommended age at initiation (in months). Graduation from medical school before 1990 (white bar) and in the 1990s (black bar) are shown. Note that those who graduated in the 1990s recommend that vitamins be initiated at later ages.
Pertussis (Whooping Cough)
Despite vaccination protocols, pediatric hospitalists continue to see whooping cough in young infants. (See Figure 1, p. 39.) Even with treatment, the damage can be severe, and the length of stay (LOS) is prolonged compared with those of most other patients with complex illnesses. “Vaccine fatigue” means that immunization lasts only until adolescence or early adulthood, at which time they need appropriate boosters. If the patient hasn’t receive boosters, the initial immunization loses its effectiveness; unprotected, they can be infected with the disease, though sometimes not badly enough for them to seek care. When they do, the diagnosis is often community-acquired mild pneumonia or a more traditional bronchitis. Either by accident or because the physician has given it thought, those illnesses are treated with a macrolide drug, which is also—coincidentally and serendipitously—the drug of choice for pertussis. But many remain carriers because they are not accurately diagnosed or never seek care.
