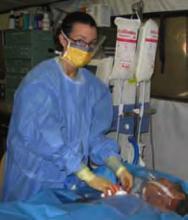
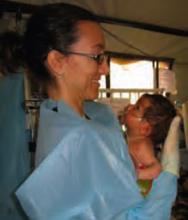
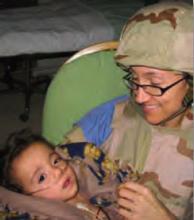
(Maj) Heather Cereste, MD, chair of the Bioethics Committee at Wilford Hall Medical Center at Lackland Air Force Base near San Antonio, Texas, and a member of Team Hospitalist, is the only geriatric-trained internist in the U.S. Air Force. From January through May 2007, she served as the attending primary care physician at Balad Trauma Hospital in Balad, Iraq. She recently spoke with The Hospitalist about her experience as a wartime physician.
Q: What motivated you to join the Air Force?
A: I talked to the Air Force near end of third year in residency. A number of things played into my decision. I was in Manhattan during 9/11 and got caught up in the surge of patriotism. I had thought about the military before, and was at a point when I was about to enter geriatrics and wasn’t sure if wanted to go into the traditional workforce or explore something else. I joined the reserves in 2004 and went active in 2006. To be honest with you, I never thought I would be deployed to a combat zone.
—Heather Cereste, MD
Q: What type of training did you receive before going to Iraq?
A: I was just undergoing the credentialing process when I was asked by my commander [to] deploy with her in a few months. I was a little shocked and taken aback, and didn’t feel at all prepared. So I inquired about further training and was referred to the shock trauma group in Baltimore, Md. It was the closest I could get to warfare type of injuries because it’s an urban warfare they fight in Baltimore. There, I was able to gain confidence in doing some procedures, including chest tubes, and refreshing myself about central lines and the acuity of care.
Q: What was it like working in Iraq?
A: Our team worked seven days a week in the intensive care unit. We were on call every fifth night, overnight. We took care of the critically ill patients who came in through ER or who were directed to us. For the most part, we interacted with the coalition people for only 24–48 hours before they were transported out. The American and British people often went to Germany for more definitive care.
Q: What medical conditions did you see?
A: Over five months we managed about 528 critically ill people. There were certainly a lot of postoperative cases. We took care of burns and head wounds, which were increasing in number, a lot of limb amputations, as well as blast injuries and gunshot wounds. Civilians would present at our gates and we could triage them, if we had enough room.
Q: Did you feel like you were in a war zone?
A: It was very surreal. I was one of the last rotations to go when it was a tent hospital, so when we had rain and weather, we’d have to deal with floods, etc. It was a very rustic environment; there was dust was everywhere. The helicopters would come in and land right outside our tents.
Our hospital was right next to the wire–that’s a barbed wire fence that separated our base from the outside of the base–so we heard machine guns constantly while we were doing our rounds. We also got mortared frequently. Disgruntled people on the other side would set up across the river. They had some Russian mortars that they would throw over to our side. Whenever we could identify that the mortars were coming over the wall, sirens would go off and we’d have to dive for cover.