It was just before 7:30 p.m. Feb. 7 when a huge explosion in the small Georgia town of Port Wentworth shook the community to its core.
It proved to be a night no one would soon forget. It also tested the young hospitalist program at Memorial University Medical Center (MUMC) in Savannah, a few miles from Port Wentworth.
At least 12 people were killed and more than 40 seriously or critically injured in the blast at the Imperial Sugar Refinery, better known to locals as the Dixie Crystal Sugar Refinery, a Savannah-area landmark for more than 100 years.
The Place to Go
MUMC is an academic medical center with a Level 1 trauma center that serves a 35-county area in southeast Georgia and southern South Carolina. It is often said that if a patient is in a serious accident, MUMC is the place to go.
We started a hospitalist program at MUMC in September 2006, with three hospitalists and an average census of four patients. We now have seven hospitalists, expanding to 10 in July, and an average census of 65. Though still a fledgling department, we grew a lot the night of Feb. 7 and played a significant role in helping disaster victims. Immediate response, flexibility, and focus were paramount in defining our reaction to the crisis. Here’s how events unfolded that difficult night:
7:30 p.m.
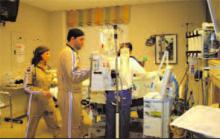
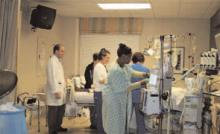
We got the call and mobilized all five hospitalists in the emergency department (ED) 20 minutes later. It was organized chaos as trauma surgeons and ED physicians attended to the rapidly increasing number of victims arriving by ambulance and helicopter. Before the blast, the ED waiting room was packed with about 45 patients who needed attention.
8:15 p.m.
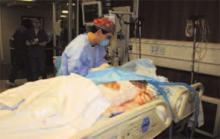
Many victims suffered serious burns from the explosion. Burn specialists from the Joseph M. Still Burn Center in Augusta arrived by helicopter. Space in the ED became desperately crowded with the seemingly endless number of victims, so we were all busily tending to the existing ED patients in every capacity possible to try and get them out of the ED. We sutured wounds, started and removed IVs, treated pregnant patients, triaged every medical patient, transported patients, and did whatever else was required. In about 90 minutes we had essentially cleared the entire ED. At this point, some of the trauma victims were moved upstairs to the intensive care unit (ICU).
9 p.m.
Victims were still arriving with burns over 40% to 80% of their bodies. After we’d cleared the ED as much as possible to make room for new patients, we focused on the immediate need for medical-surgical beds. MUMC was almost at capacity before the explosion, and suddenly a large number of patients were being emergently triaged out of the ICUs to make way for the burn victims.
The teamwork throughout the hospital was amazing to watch. From the ED to the medical floor, everyone worked together with precision as if this happened every day. Several patients were held in the ICU awaiting helicopter fight to the Augusta Burn Center; extra staff were assigned to those patients. Patient-care technicians began taking water and blankets to family members who had arrived at the hospital.