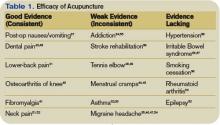
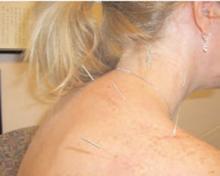
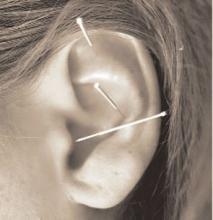
In 2004, 370 of 1,394 reporting hospitals offered some complementary alternative medicine (CAM) services in the U.S. Of the 370 hospitals reporting CAM services, 11.5% (42 hospitals) reported inpatient acupuncture services.1
This threefold increase since 1998 demonstrates the growing use of and demand for acupuncture services in hospitals. This trend is driven by patient demand and clinical effectiveness. Acupuncture is a safe treatment modality hospital physicians should be familiar because it can benefit patients in the inpatient setting.
Origins of Acupuncture
The first use of acupuncture is not known. The earliest medical textbook on acupuncture was The Medical Classic of the Yellow Emperor, written about 100 B.C. The first translation of this text into English was in 1949.2
The book outlined the theory of a system of six sets of symmetrical channels on the body’s surface, which it called meridians; along these, it posited an intricate network of points.3 Needling the points was supposed to manipulate or release the flow of energy or life force—Qi—to the internal organs, thereby alleviating symptoms. Heating acupuncture points with burning herbs—moxibustion—was also purported to relieve pain.
Acupuncture in the U.S.
The first documented use of acupuncture in the United States occurred in the 19th century. In 1826, Bache used it to treat lumbago.4 During that same era, William Mosley used acupuncture to treat patients with lumbago and sciatica.5
In 1971, a first-person account of the use of acupuncture by New York Times reporter James Reston excited great interest in the technique. Reston was introduced to the procedure to relieve pain after an emergency appendectomy during a trip to China with Henry A. Kissinger.6
Since then, there has been a steady increase in the use of acupuncture by physicians. The American Academy of Medical Acupuncture, the only physician-based acupuncture society in North America, was formed in 1987; in 1992, the Office of Alternative Medicine was created within the NIH. In November 1997, the Food and Drug Administration (FDA) removed the experimental designation for acupuncture needles and approved their use by licensed practitioners. By 1993, the FDA had a record of more than 9,000 licensed acupuncturists, estimated to be providing more than 10 million treatments annually at a cost in excess of $500 million.7
Acupuncture is part of the quasi-medical area of complementary and alternative medicine, whose practitioners field more visits annually than all primary-care physicians in this country combined.8 Most acupuncturists practice the Chinese technique.9
Licensing requirements vary by state.10 As acupuncture has gained popularity and respect, and as its benefit for various medical conditions has been proved in high-quality studies, many well-established medical institutions and universities have begun to integrate it with more traditional Western medical treatments.
Acupuncture Theories
The early Chinese theories about how best to perform acupuncture were varied and sometimes conflicting.11 Early treatments using heat, bloodletting, and crude stone implementation evolved over centuries into the intricate practice known today.