Skillful use of intravenous pain medications can be a powerful tool in the clinician’s pain management armamentarium. Yet many physicians are uncomfortable prescribing IV pain medications, especially opioids, even when their patients are experiencing severe pain—7-10 on the verbal analogue scale (VAS). This reticence, say the palliative care specialists interviewed for this article, may be due to a lack of training and knowledge, as well as misperceptions about proper use of IV opioids. The end result for patients can be inadequate pain control, which, according to researchers, continues to be a problem in U.S. hospitals.1
Even hospitalists not affiliated with a surgical service who do not treat perioperative patients are likely to encounter many different scenarios in which IV pain medications could appropriately address patients’ discomfort. David Ling, MD, a member of SHM’s Palliative Care Task Force, a hospitalist at Baystate Medical Center in Springfield, Mass., and assistant professor of medicine at Tufts University School of Medicine (Boston), says patients who need IV pain medicines range from those with acute abdominal pain, pancreatitis, or small bowel obstructions to patients with end-stage cancer, renal disease, or congestive heart failure.
“It’s probably a bigger number on the medical service than most people realize,” he says.
The Short List
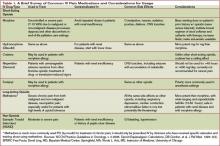
When it comes to effective IV pain medications very few choices exist, according to recommendations from the National Comprehensive Cancer Network and other pain advocacy organizations. An informal poll of interview sources corroborates this revelation.
“Morphine is the gold standard in pain control,” says Thomas Bookwalter, PharmD, clinical pharmacist on the General Medicine Service at the University of California at San Francisco (UCSF) Medical Center, a Health Sciences associate clinical professor at the UCSF School of Pharmacy, and a member of SHM’s Palliative Care Task Force.
Preferences for morphine or other opioids vary by practitioner and institution. For instance, says Dr. Bookwalter, the pain service at UCSF has been using hydromorphone more frequently of late.
Nicole L. Artz, MD, director of the Adult Sickle Cell Disease Care Team at the University of Chicago Hospitals and instructor of medicine at the University of Chicago Medical School, also occasionally uses IV infusions of ketorolac—a powerful NSAID designed for short-term management of moderately severe pain in adults. But, like morphine, it is contraindicated in patients with renal insufficiency and can have GI side effects.
Common Missteps
That opioids remain the drugs of choice for controlling severe pain puts some physicians outside their comfort zone. Dr. Ling, who has extensive experience with IV opioids, has observed two common tendencies among physicians inexperienced with prescribing opioids. “There is a tendency, based on the traditional teaching, to prescribe a lower-than-necessary first dose and for those doses to not be frequent enough,” he says.
Dr. Artz, who has a special interest in pain management, lectures on effectively using opioids to house staff at the University of Chicago. She has observed a deficit in physician training in pain management and has seen physicians make many errors when writing orders for opioids, including mixing IV and short-acting oral opioids or two long-acting opioids, not distinguishing between patients who are opioid-naïve and opioid-tolerant in choosing a starting dose, failing to titrate short-acting opioids rapidly despite inadequate pain control, and giving orders for repeated doses of morphine in patients with renal insufficiency.
Dr. Bookwalter says the World Health Organization’s stepladder approach to treating pain (starting with oral NSAIDs and moving up to opioids) does not align with current scientific thinking on prescribing pain medication. For severe pain, a clinician should consider immediately starting an IV opioid, reassessing the patient every 15-30 minutes to see whether the dose is effectively decreasing the pain. National Comprehensive Cancer Network (NCCN) Guidelines for Adult Cancer Pain recommend rapid dose escalation to address the level of the patient’s pain.2