In June the Centers for Medicare and Medicaid Services (CMS) issued a notice proposing changes to the Medicare Physician Fee Schedule (MPFS) that, if enacted, would significantly increase Medicare payments to hospitalists for many services routinely performed. Because many private health plans use the Medicare-approved RVUs for their own fee schedules, it is anticipated that hospitalists will likely see payment increases for their non-Medicare services as well.
The changes, which will take effect in January 2007 if enacted, reflect the recommendations of the Relative Value Update Committee (RUC) of the American Medical Association, along with input from SHM. At this point, however, they are only proposed changes that CMS could modify based on input from affected groups and Congress. SHM will continue to urge CMS to implement the proposed changes and we encourage all hospitalists and other interested individuals to send a letter to CMS indicating support for the proposed changes. (See “How to Show Your Support,” p. 15.) CMS is accepting comments on the rule until August 21, with the final ruling expected in November.
The suggested revisions—the largest ever proposed for services related to patient evaluation and management—are designed to improve the accuracy of payments to physicians for the services they furnish to Medicare beneficiaries. The proposed notice includes substantial increases for “evaluation and management” services (that is, time and effort that physicians spend with patients in evaluating their condition and advising and assisting them in managing their health).
The proposed notice addresses two components of physician payments under the MPFS:
- A comprehensive review of physician work RVUs; and
- A proposed change in the methodology for calculating practice expenses.
“Medicare law requires CMS to assess the accuracy of the work relative values it assigns to physician-services every five years,” says SHM CEO Larry Wellikson, MD. “SHM, on behalf of our members, participated in a coalition of internal medicine groups, led by the American College of Physicians, which provided survey data and other evidence to the RUC to show that many services were undervalued compared to other physician services and that it was essential that their work RVUs be increased.”
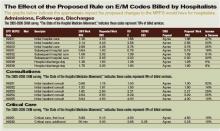
Consistent with the RUC’s recommendations, CMS is proposing the largest increase in the work RVUs assigned to office and hospital visits and consultations since Medicare implemented its physician fee schedule in 1992. Many of these reflect double-digit increases for codes commonly billed by hospitalists:
- The work RVU for initial hospital care (CPT code 99221) would increase by 47%;
- The work RVU for subsequent hospital care (CPT code 99232) would increase by 31%; and
- The work RVU for subsequent hospital care (CPT code 99233) would increase by 32%.