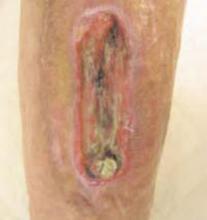
Despite modern wound treatment and broad-spectrum antibiotic treatment, patients with chronic wounds still exist. The appearance of antibiotic resistant bacteria, such as methicillin-resistant Staphylococcus aureus (MRSA) in the 1980s and ’90s, gave rise to a search for other remedies. One of the remedies that has been rediscovered and subsequently successfully reintroduced is maggot debridement therapy (MDT).1 The fact that more than 100 articles were published on the subject in the past two decades indicates that the use of maggots is making a strong comeback in medicine.2 In January 2004, the U.S. Food and Drug Administration (FDA) issued 510(k)#33391, allowing production and marketing of maggots as a medical device. In this article, we discuss the use of MDT in patients with a chronic wound.
A Long History of Maggot Therapy
MDT has been used in many cultures and has been known for centuries.3 Ambroise Parè is credited as the father of modern MDT. Unfortunately, no evidence can be found of Parè using maggots as a means to clean or heal wounds. The only reference is the often-cited case that occurred in 1557 at the battle of St. Quentin, when Parè observed soldiers whose wounds were covered by maggots. He mainly described the negative effects of the maggots, and, above all, believed they were spontaneously produced by the wound itself, not by the eggs of fly.4
Baron Larey (1766-1842) a famous surgeon in the army of Napoleon Bonaparte, wrote about soldiers who had larvae-infested wounds, but was frustrated that it was difficult to persuade his patients to leave the maggots in place, believing that “they promoted healing without leaving any damage.”5
The first surgeon to use MDT in patients in the hospital was the orthopedic surgeon William Baer. In the 1920s he was faced with a group of untreatable patients with severe osteomyelitis (antibiotics had not yet been discovered). He successfully treated many patients with maggots, and because of his success the therapy became regularly used in the United States.6
By 1934 more than 1,000 surgeons were using maggot therapy. Surgical Maggots were available commercially from Lederle Corporation.7 But with the introduction of antibiotics in the 1940s, the use of maggots dropped off. In the following years, case reports were published only occasionally.
The Negative Image of Maggots
A large problem of MDT is the difficulty of this type of therapy to gain acceptance in the medical community. Maggots are associated with rotting and decay. The image is of filthy, low-life creatures that are ugly and disgusting. Although a nice recent example for the general public is the scene in the movie Gladiator. The main character (played by Russell Crow) is advised to leave the maggots that spontaneously infested a wound on his shoulder in place so that the wound would heal. He leaves them in place and the wound heals without any problem, enabling Crow’s character to fight many battles.
In contrast, in an oral presentation we held recently at a Dutch scientific surgical meeting, a surgical professor in the audience said, “I will never allow those creatures in my ward.”8 This remark shows that widespread use and acceptance of MDT has not yet been reached. It seems there is still much work to do before MDT is generally accepted as a therapeutic method.
Fortunately, the negative image that seems to exist among nurses and physicians does not seem to bother patients.9 We have treated more than 100 patients in our clinic with MDT. All patients to whom we proposed MDT agreed to the therapy. All were allowed to discontinue the therapy whenever they wanted; none did. In a survey of the first 38 MDT-treated patients, 89% agreed to another session of MDT if the surgeon believed it would be beneficial, and 94% of the patients said that they would recommend it to others. This is despite the fact that the therapy was not successful in all patients (there was a below-knee of above the knee amputation-rate of 19% among patients who underwent MDT).10