A24-year-old white female is admitted directly to the hospital by her cardiologist for a wound infection. She is a medical technology student who underwent a pacemaker implantation three weeks prior for persistent symptomatic bradycardia. She now complains of pain, redness, and swelling at the site of her pacemaker incision site. She reports fevers, chills, night sweats, and multiple other systemic symptoms.
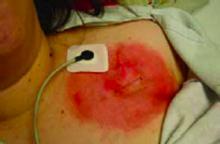
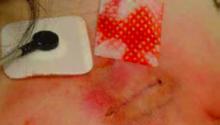
On physical exam, she appears quite pleasant, in no apparent distress, and without any abnormalities in vital signs. Her incision site reveals an erythematous, geometric, annular patch with no edema, warmth, induration or discharge. (See photo.)
What is the most appropriate treatment for this patient?
- Draw blood cultures, place central line, and begin broad-spectrum antibiotics.
- Draw blood cultures, place central line, and begin broad-spectrum antibiotics and also itraconazole to cover atypical mycobacteria infection.
- Schedule surgery to remove pacemaker.
- Gently approach patient about stressors and possible underlying psychiatric issues and consult psychiatry.
- Obtain wound cultures and apply mupirocin ointment twice daily.
Discussion
The correct answer is D: Gently approach patient about stressors and possible underlying psychiatric issues and consult psychiatry.
This patient had been applying an external agent (most likely makeup) to her wound site. On questioning, the patient and her family continued to deny any manipulation of the wound even when the substance was wiped away with an alcohol pad. (See photo above.) Additionally, a half-empty bottle of clonidine was found under her pillow. The clonidine was apparently used as an attempt to feign hypotension. She denied taking the medication, but the medical team suspected that the use of these antihypertensives led to her previous symptomatic bradycardia and eventual pacemaker implantation.
Despite gentle questioning and evaluation for stressors and signs of depression, the patient left the hospital against medical advice before psychiatric consult could be obtained. The patient eventually returned to the cardiology clinic complaining again of wound infection. A wound culture revealed Enterococcus faecalis consistent with fecal contamination of her incision site. Eventually, her pacemaker was removed. She did continue to see different physicians and visit different hospitals before being permanently lost to follow up.
This case of Munchausen syndrome demonstrates many of its defining characteristics. Munchausen syndrome was originally described by Asher in 1951 in Lancet. Its name is derived from Baron von Munchausen, a German nobleman who told humorous but outlandish tales about his travels, including riding on cannonballs, traveling to the moon, and discovering an island made of cheese. Munchausen syndrome is a factitious disorder (symptoms are intentionally produced), but unlike malingering there is no apparent secondary gain except to satisfy the psychological need to receive attention or support. These patients often undergo medical evaluations and multiple, invasive, surgical procedures simply to have them. The DSM-IV points out that the motivation for the behavior is only to assume the sick role.
Patients tend to be young adults and are more often male. They may describe and have physical findings of any number of illnesses. They may have undergone many prior surgical procedures and have several scars on physical exam. Classically, they have seen several different physicians and often have some medical knowledge including medical terminology.
Treatment is often difficult. It is appropriate to address any possible underlying organic disease by systemic approach to avoid overlooking any dangerous conditions. If none is found, the patient should be assessed for stressors, signs of psychosis or depression, and any possible financial or other secondary gains. It is important to recognize Munchausen syndrome as a factitious disorder as opposed to a somatoform disorder (somatization, conversion, hypochondriasis). A factitious disorder is produced artificially by the patient, whereas symptoms of a somatoform disorder are not under the patient’s control. TH