In 2002, the NIH surveyed more than 30,000 U.S. adults regarding their use of complementary and alternative medicine (CAM).1 This survey revealed that approximately 40% of U.S. adults had used some form of CAM in the past year. When one excludes prayer as a CAM modality, the most common modality used was the category of natural products (i.e., herbs and dietary supplements).
This has significant implications for all healthcare providers, but especially for those who practice in the hospital environment. Herbs can be potentially toxic in their own right and can cause drug-herb interactions as well. Such adverse effects may be particularly important in hospitalized patients undergoing surgery or who are acutely ill and exposed to a number of narrow-window therapeutic pharmaceuticals. Thus, it is imperative for hospital physicians to have a basic understanding of some of the risks, challenges, and potential benefits of herbs.
Use of Herbs by Hospitalized Patients
Surveys performed in the United States and around the world consistently demonstrate that the use of dietary supplements and herbs tends to be higher (as is all CAM usage) in individuals with chronic or incurable diseases. This is especially true for conditions such as HIV, diabetes, heart disease, and cancer.2–6 Thus, considering the complexity of illness of most hospitalized patients, it should not be surprising that use of herbs and dietary supplements is high in the hospital population. This has been borne out in several national and international studies.
A study reported in the Annals of Emergency Medicine in 2000 found that 56% of ED patients had tried alternative therapies in the past.7 The most frequently tried alternative therapies were massage therapy (31%), chiropractic (30%), and herbs (24%). Interestingly, 70% of the respondents who had tried these alternative therapies did not inform their physicians, highlighting a challenge for physicians and caregivers in the hospital setting.
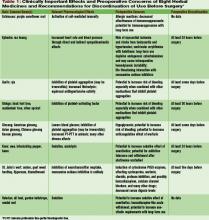
Kay and colleagues reported 1,017 patients presenting for a preanesthetic evaluation prior to surgery.8 They found that 482 of 755 (64%) of patients had used at least one natural product. The majority of these were vitamin users, but several herbs with potential importance in the hospital setting were used as well: garlic extract (43%), ginkgo (32%), St. John’s wort (30%), ephedra (18%), and echinacea (12%).
Pediatric patients are not immune to the use of herbs and dietary supplement either. A survey at Children’s Hospital in Boston looked at 1,100 patients younger than 18 during their preoperative visit.9 A total of 1,021 surveys were completed and, of these, 30% patients indicated that they had tried one or more complementary and alternative therapies in the past year before surgery. Importantly, 13% had used herbal remedies before surgery.
Finally, international studies confirm similar usage patterns in adult hospital patients in Germany, Spain, Hong Kong, and Australia.10–13 Thus, it appears well established that the use of dietary supplements has become a fixed part of conventional healthcare. Recognizing that a significant percentage of patients under our care are using herbs is the first step in bringing critically needed information and guidance to our patients.
Herb Toxicity and Herb–Drug Interactions
There are many well-recognized herbal toxicities and/or drug-herb interactions with which all clinicians should have some degree of familiarity. For example, St. John’s wort stimulation of the cytochrome P450 enzyme system resulting in enhanced metabolism of several pharmaceutical drugs has been well reported. Ephedra’s ability to induce elevated blood pressure, stroke, and MI also received a great deal of publicity. (Note: Ephedra sales were banned by the FDA in 2004. However the prohibition excluded ephedra-containing teas, and—despite the ban—many internet sites still have ephedra available for purchase. Thus, be aware that your patients may still have access to ephedra.)