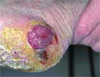
An 85-year-old female developed a sore on the left foot (see image above) during the past six months. Throughout that time she underwent periodic debridement and local wound care with gentamicin ointment followed by the use of silver sulfadiazine cream dressings, an Unna Boot, and a surgical shoe with heel relief. Despite treatment her wound increased in size, bleeds easily, but it is not painful.
WHAT IS YOUR DIAGNOSIS?
- Pyogenic granuloma;
- Squamous cell carcinoma;
- Amelanotic melanoma;
- erkel cell carcinoma; or
- Hypertrophic granulation tissue?
Discussion
The correct answer is C: amelanotic melanoma. The patient’s skin biopsy revealed a nodular malignant melanoma with ulceration, Clark’s level V, Breslow thickness at least 5.8 mm. She underwent wide local excision with sentinel lymph node biopsy, which was negative for tumor. The defect was repaired with a split-thickness skin graft and temporary wound vacuum. She is being closely monitored for local recurrence and in-transit metastasis.
Melanoma classically presents as an asymmetric, irregularly hyperpigmented lesion with ill-defined borders; however, some melanomas have little to no pigment and can be easily confused with other benign or malignant entities. Amelanotic melanomas comprise about 2% to 8% of all melanomas.1-2 A seemingly amelanotic lesion may have an area of subtle pigmentation peripherally that can be a clue to the diagnosis.2-3 The prognosis of amelanotic melanomas is the same as that of pigmented melanomas and is contingent upon depth of invasion, location, and patient age and gender. Unfortunately, the diagnosis of an amelanotic melanoma is often delayed, leading to more advanced tumors. Treatment is analogous to pigmented melanomas.2
A rapidly proliferating amelanotic melanoma can be clinically confused with a pyogenic granuloma, a benign vascular hyperplasia. Pyogenic granulomas present as solitary, discrete, erythematous papules or pedunculated growths on cutaneous and mucosal surfaces. They are often friable and may ulcerate. Pyogenic granulomas are more common in children and young adults, but they can occur at any age. If a pyogenic granuloma is not surgically excised, its growth will eventually stabilize, leading to involution, necrosis, or shrinkage to a fibrotic papule.4
Hypertrophic granulation tissue is another benign entity that can resemble an amelanotic melanoma. The production of granulation tissue is a normal response in the early proliferative stage of wound healing. Granulation tissue has abundant vascular structures, which give it an erythematous, edematous, and friable appearance. As wound healing progresses, granulation tissue is replaced with new epidermis through re-epithelialization.5 Failure of a wound to show signs of progressive healing should prompt a biopsy to distinguish normal granulation tissue from malignancy. Amelanotic melanoma has been reported in cases of nonhealing diabetic foot ulcers.6
Amelanotic melanoma can also be difficult to clinically distinguish from other malignant growths, such as squamous cell carcinoma. More common in elderly patients, squamous cell carcinoma commonly presents as a pink to erythematous, scaly papule, or plaque on a sun-exposed surface. Treatment of superficial squamous cell carcinoma, such as Bowen’s disease, with cryotherapy or cautery is highly effective; however, if an amelanotic melanoma is mistakenly treated as Bowen’s disease, then the delay in eventual histological diagnosis may result in an advanced stage amelanotic melanoma.7
Merkel cell carcinoma is a highly aggressive tumor that typically presents as an erythematous to violaceous, painless, solitary nodule or plaque that grows rapidly. It usually affects older patients and commonly occurs on the head. It has a high likelihood of local recurrence, metastasis, and poor prognosis.8 Merkel cell carcinomas are rare, and they elicit the same differential diagnoses as amelanotic melanomas. Histological differentiation from amelanotic melanoma is necessary. TH