Pneumonia is associated with as many as 2 million annual deaths among children globally and 19% of all deaths in children less than 5 years of age (1). It is one of the most common diagnoses made in the acutely ill child, with an annual incidence of 34 to 40 cases per 1,000 children in Europe and North America.
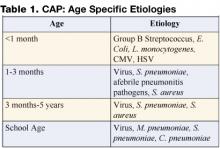
In the past, viral pathogens were estimated to cause as many as 80% of cases. Streptococcus pneumoniae was generally regarded as the most frequent bacterial cause of community-acquired pneumonia (CAP), especially in cases with complicated parapneumonic effusions. Infectious etiologies are age specific, with bacterial etiologies predominating in the very young infant and viral pathogens in the older infant and adult (Table 1). Knowledge of the most likely pathogen, the prevailing susceptibilities of these infecting pathogens, and the severity of the illness will help guide antibiotic and other treatment decision making.
Most children do not require hospital admission, and mildly ill children who likely have a viral illness do not need antibiotics. The following guideline will attempt to help the practitioner identify those who do require hospitalization and provide an approach to management of those with complicated infection.
Recognition of the Patient with CAP
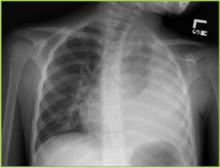
The first obstacle is to identify the patient with pneumonia. In managing the child with CAP, it is important to distinguish those with other underlying pathology, including asthma, RSV, or other confirmed viral etiology. It is important to remember that pathogens in the compromised host, cystic fibrosis patient, or patient with other chronic pulmonary pathology are different from typical CAP pathogens and include a wide differential. Most patients with CAP have an acute illness associated with fever (>38°C), cough, and evidence of lower respiratory tract symptoms/signs. Chest radiograph typically shows pulmonary infiltrate. Whether this is patchy infiltrate or lobar in appearance can assist the practitioner in treatment decision making in that the latter is much more likely to be associated with a bacterial etiology.
Once the diagnosis is considered, further assessment should focus on hydration status, hemodynamic parameters, and oxygenation. A careful assessment should identify other associated foci (i.e., meningitis or bacteremia) on examination and laboratory evaluation.
Identification of the Patient Requiring Hospitalization
Consider hospital admission for the toxic patient, those with altered mental status, significant dehydration, hypoxemia, dyspnea, grunting respirations, or retractions, and any patient with hemodynamic instability. Chest radiograph showing a significant pleural effusion should also be considered an indicator for hospital admission.
Bacterial pathogens are more likely in the severely ill patient, patients with a rapidly progressive process, and those with radiographic evidence of lobar consolidation or pleural effusion. Some children with viral processes may require admission for supportive care.
Prompt Recognition of the Patient with Empyema
For the patient with pneumonia and parapneumonic effusion, distinction between a free-flowing effusion and pleural empyema is critical. Standard plain film can identify pulmonary infiltrate and often effusion and lateral decubitus films can help identify free flowing effusion (Figure 1). While CT scan more effectively identifies pleural fibrinous adhesions that may entrap lung, ultrasound most effectively identifies complex fluid collections with loculation and septation, and it can be utilized to guide thoracentesis.
Empyema is defined as pus in the pleural space and is estimated to occur in 10–40% of patients with pneumonia. Empyema may also result from causes other than a complication of bacterial pneumonia, such as thoracic trauma or postsurgical complication, rupture of lung abscess, esophageal tear, or complication of indwelling catheter. It generally occurs in stages including acute (early-cloudy fluid), fibrino-purulent (thicker, multiloculated fluid), and organized (late with thick pleural peel and entrapment of lung).