Joel Barker describes leadership as “…the ability to take people where they otherwise would not go.” In other words, leadership is about creating change in something that exists today. Management, on the other hand, may be considered a series of steps to ensure that things happen the desired and consistent way. Although this article is not of scope sufficient to explore the differences between management and leadership, it will address a domain in which the 2 intimately intersect. Managing others relies upon many foundations of leadership, such as establishing the group’s vision and setting key strategic goals. In like manner, successful leadership in stimulating change is dependent on the effective management of personnel to ensure that the culture, work habits, outcomes, and behaviors are consistent with the change efforts. This article will focus on the management of physicians in hospital medicine groups. The 8 steps outlined are applicable regardless of employer type, group size, or mission. Almost all of the skills necessary to effectively implement a performance management system can be learned and are best practiced on a regular basis. Furthermore, there are many existing resources for further education and development in these areas based on one’s current level of competency.
The author wishes to acknowledge the faculty of the American College of Physician Executives for their work in assembling many of the concepts found in this article. The course “Managing Physician Performance in Organizations” serves to underscore an integrated model of performance management and explores some of the theoretical bases of human behavior not included here.
Defining Your Group
Before you can manage performance, you must know the parameters by which the group is defined. The prerequisites for performance management include salient statements of mission, vision, and values. The mission defines the purpose for the group being in place and usually reflects the interests of the hospital(s) or medical group affiliated with or actually employing the hospital medicine group. The mission statement should be able to answer the questions “Why does our hospital medicine group exist? What purpose does it serve? In very broad terms, what scope of services do we provide?” The vision is a concise summary of what the group would like to be or achieve in the future, and it may relate to growth, range of services, outcomes, or other dimensions. Most often the vision is the leader’s platform for change in order to articulate the rationale for creating a better future. Values are those characteristics that guide decision making and provide guidance for everyone’s expected behavior and conduct in the group. Values can be thought of as the “lens” through which the vision is carried out and the mission upheld.
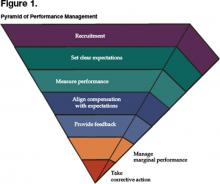
From the mission, vision, and values come strategies for achieving successful change and the more specific goals that the group is to attain. In some cases the group may have undertaken a formal strategic planning process that rendered a series of goals, objectives, and/or programs to be carried out in the immediate to intermediate term. We now reach the vital area in which a well structured and supported performance management system can play a pivotal role in ensuring the successful implementation of strategic thinking. Until now, the thought and planning process had focused on the right thing to do. From here, the focus becomes doing things right. Once you have completely answered the questions above and have a confident sense of where your group is heading and why, then the steps that follow will enable you to stack the deck in favor of achieving the level of performance you desire. Note that each step is embedded in action. Figure 1 represents the pyramid of performance management, a prioritized approach to managing others.