Case
A 45-year-old woman was admitted with choledocholithiasis. Two days prior, following endoscopic retrograde cholangiopancreatography (ERCP), she had gone to the OR for cholecystectomy. The procedure was completed laparoscopically, though the surgeon reported a difficult dissection. The surgeon left a Blake drain in the gallbladder fossa, which initially contained punch-colored fluid. Today, there is bilious fluid in the drain.
Overview
Surgical drains are used to monitor for postoperative leaks or abscesses, to collect normal physiologic fluid, or to minimize dead space. A hospitalist caring for surgical patients may be the first provider to note when something changes in the color or volume of surgical drains. Table 1 lists various types of drains with their indications for use.
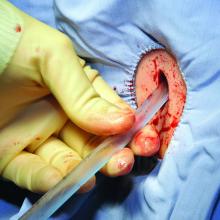
Lung re-inflation after surgery, using a chest drain. The lung was originally collapsed to allow access to the chest organs during surgery. The lung collapse was done by opening up the pleural cavity to air from outside. The lung re-inflates naturally when this air is withdrawn using the chest drain being inserted here.
Surgical Tubes and Drains
Chest tubes. Chest tubes are placed in the pleural space to evacuate air or fluid. They can be as thin as 20 French or as thick as 40 French (for adults). Chest tubes are typically placed between the fourth and fifth intercostal spaces in the anterior axillary or mid-axillary line; however, the location may vary according to the indication for placement. The tubes can be straight or angled.
The tubes are connected to a collecting system with a three-way chamber. The water chamber holds a column of water, which prevents air from being sucked into the pleural space with inhalation. The suction chamber can be attached to continuous wall suction to remove air or fluid, or it can be placed on “water seal” with no active suction mechanism. The third chamber is the collection chamber for fluid drainage.
Indications for a chest tube include pneumothorax, hemothorax, or a persistent or large pleural effusion. Pneumothorax and hemothorax usually require immediate chest tube placement. Chest tubes are also commonly placed at the end of thoracic surgeries to allow for appropriate re-expansion of the lung tissue.
A chest X-ray should be obtained after any chest tube insertion to ensure appropriate placement. Chest tubes are equipped with a radiopaque line along the longitudinal axis, which should be visible on X-ray. Respiratory variation in the fluid in the collecting tube, called “tidling,” should also be seen in a correctly placed chest tube, and should be monitored at the bedside to reassure continued appropriate location. The interventional radiologist or surgeon who placed the tube should determine the subsequent frequency of serial chest X-rays required to monitor the location of the chest tube.
If the patient has a pneumothorax, air bubbles will be visible in the water chamber; called an air leak, these are often more apparent when the patient coughs. The chest tube should initially be set to continuous suction at -20 mmHg to evacuate the air. Once the air leak has stopped, the chest tube should be placed on water seal to confirm resolution of the pneumothorax (water seal mimics normal physiology). If, after the transition from suction to water seal, resumption of the air leak is noted, it may indicate recurrence of the patient’s pneumothorax. A stat chest X-ray should be obtained, and the chest tube should be placed back on continuous suction. In general, a chest X-ray should be obtained any time the chest tube is changed from suction to water seal or vice versa.
thank you, very helpful quick read.